For the overwhelming majority of patients that have low back pain, the pain is short lived. The irony is that because of this fact most physicians give the treatment of low back pain short rift. A fundamental assumption is made that the back pain will improve regardless of the treatment recommended. The physician can prescribe the proverbial, “Take two pills and call me in the morning”, treatment. However, there are millions of low back pain sufferers for whom back pain is still there the next morning.
In fact, not only is the pain there the next morning, it is there the next week, the next month, and possibly even the next year. It is this group of individuals, in particular, for whom proper diagnosis, including the appropriate radiological studies are key in making the diagnosis. It is also this group of patients who frequently seek both conventional Western, as well as alternatives, sometimes referred to as Eastern integrative treatment options. What further complicates the issue is that for those patients who do develop chronic low back pain, a diagnosis in most instances is difficult or almost impossible to make.
Chronic low back pain is usually defined as pain that lasts longer than would be predicted, based on a comparison with other patients with the same symptoms in whom the pain has already disappeared. Some include in the definition the fact that in most chronic pain patients, the exact etiology or source of the pain is not discovered. This is not to say that these patients don’t have pain. It may be more a reflection that our present day imaging techniques are inadequate to demonstrate pathology of soft tissues that would explain the patient’s symptoms.
What this means is, that there are hundreds of thousands of individuals in the U.S. who have chronic low back pain whose diagnostic studies, physical exams and neurological exams are normal. In this context, a neurological exam means that they have normal strength, normal sensation, and normal reflexes. What they may not have is normal flexibility, mobility and /or agility of their spine. In part, this is because activity causes pain and because the activities themselves are limited by the nature of the pathological process.
So, what do we do?
Many of these patients will respond to medication, including non-steroidal anti-inflammatory, which sometimes can be taken by low back pain patients on a continuing basis. A smaller number of patients will end up with a long-term use of narcotic analgesics. The latter is something that most physicians, including myself prefer not to prescribe.
Many patients also benefit from courses of physical therapy, trigger point injections, epidural steroid injections, and other more invasive, but nonsurgical modalities. In addition, there are surgical modalities that particularly address the needs of chronic pain patients, including the placement of dorsal column stimulators and morphine pumps.
Most chronic pain patients do not significantly benefit from the types of surgical spine procedures reserved for non-chronic patients and those would include discectomy, laminectomy and fusion procedures.
But what about those individuals who might benefit from integrative therapy or what some would describe as “alternative therapy?” In my own practice, I have had tremendous success with a number of treatment modalities. However, before describing them, it is useful to review the treatment goals.
Treatment goals
When I consider patients for integrative or non-integrative treatments, my goals for them are the same and include:
1. Reduction in pain.
2. Increase in the patient’s flexibility and mobility.
3. Have the patient learn proper body mechanics. This is important because improper body mechanics may lead to poor posture. Misuse of body mechanics is a frequent cause of acute and chronic low back pain, and by incorporating treatment modalities that teach the patients efficient body mechanics, they will become more self-reliant.
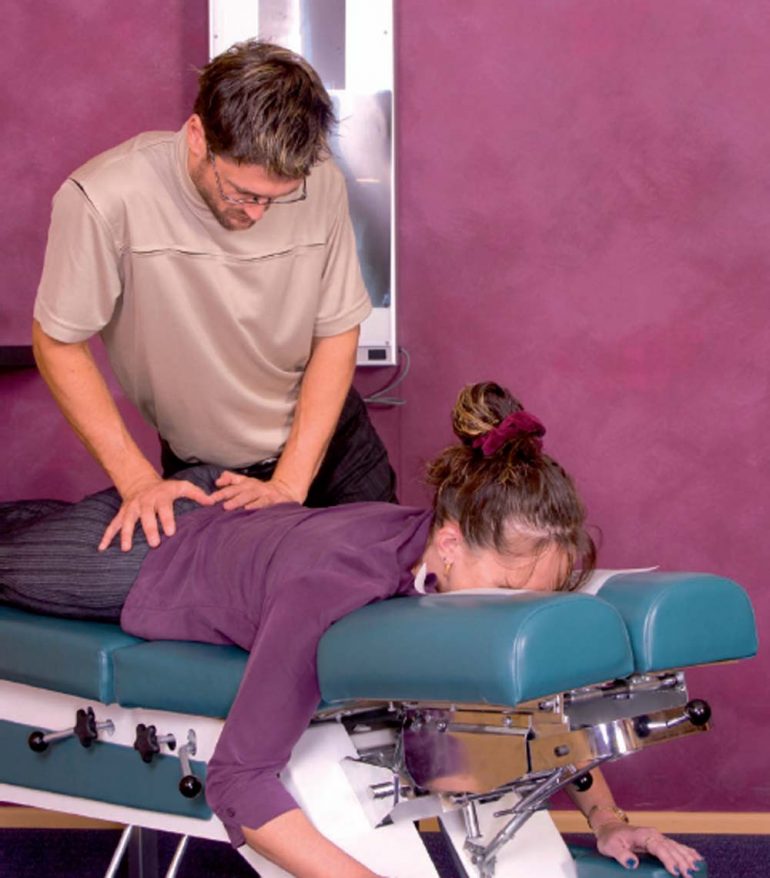
The modalities that I found most effective in my practice in terms of reducing the pain are chiropractic care, as well as acupuncture. In many instances, chiropracty is no longer considered an integrative treatment therapy because it is so widely used and accepted as a mainstream modality.
Chiropractic care is for many an effective treatment therapy, especially when the diagnosis of abnormality in the joints of the spine is diagnosed. It is challenging, however, for these patients who get only chiropractic care to maintain the pain-free state and patients frequently need to come back to the chiropractor numerous times for additional treatments. I have also found that a trial of acupuncture in the hands of a qualified acupuncturist frequently gives long-lasting relief and enhances chiropractic care.
As far as flexibility and mobility are concerned, I have seen terrific results with the patients using yoga alone, or in combination with Pilates technique. Not only do these two techniques challenge the individual to increase their ability to stretch and to strengthen, but at the same time, many individuals who take on this regimen will lose weight and will strengthen their abdominal core muscles. In some respect, this is a secondary effect, but in many respects it is a primary positive result of these treatment modalities.
A large number of my patients also found benefit from using the Alexander Technique. The Alexander Technique is a mind-body approach that teaches the individual how to find useful posture by learning to realign the spine, so activities can be pain-free.
I have seen the Alexander Technique used successfully in individuals who have what I described as “repetitive spinal strain syndrome”. More specifically, in my practice the patients who have abnormal spinal use may benefit from the Alexander Technique. By teaching the patient effective body mechanics – what I sometimes think of is a natural biofeedback system – these patients become pain-free. With lessons, the patient can learn how to effectively align themselves in this position, without the necessity of a teacher being present.
In summary, these integrative modalities are the ones that I found most beneficial for my own patients. In fact, as a back pain sufferer, I have used them effectively myself. This is meant in no way to suggest that other treatment modalities are less effective, but for the treatment modalities that I have suggested, there is evidence-based research of their effectiveness. I would hope that more and more of the integrative treatment modalities would be submitted to clinical trials to demonstrate their effectiveness.
The last point I would like to make is the case for consistency. I am sympathetic to those patients who find that they try one of these integrative treatments, do very well with them and once they are doing well, slack off and discontinue with the practice regimen. I am sympathetic because I myself have a tendency to stop when things are good and find all sorts of excuses not to do my back pain exercises, my stretching, yoga, or Alexander lessons when I am feeling well. Like most of my patients, I am working on it and I am constantly striving to maintain my weight and support my core musculature. Ultimately, these are the modalities that will be effective in my treatment and the treatment of my patients.
If you find that you have chronic back pain, I always recommend that you first have a comprehensive medical workup to assure yourself that you do not have a serious condition. Once that has been accomplished, do some research, sit down with your doctor and determine which of the treatment modalities may best be suited to relieve your pain.